COVID-19 May Be Associated with Digestive Symptoms
- by Dr. Daniel
- Published on
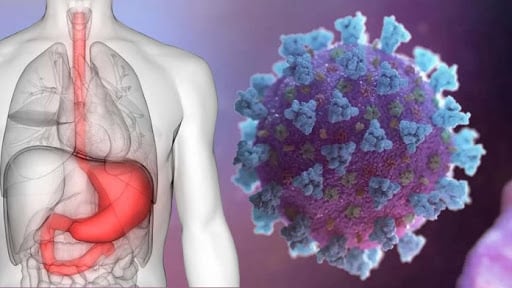
Digestive symptoms were common in patients with COVID-19, according to the American Journal of Gastroenterology.
Patients with these symptoms had a longer time from onset to admission and their prognosis was worse compared with patients without symptoms.
Key Findings of This Study
- Compared to COVID-19 patients without digestive symptoms, those with digestive symptoms have a longer time from onset to admission and a worse clinical outcome according to this analysis by investigators from several hospitals and research centers in China who gathered data on 204 patients with COVID-19 presenting to three hospitals in Hubei province from January 18, 2020 to February 28, 2020. Diagnosis was confirmed by real-time RT-PCR. Clinical characteristics, laboratory data and treatment information for the patients were included in the final analysis.
- Of the 204 patients, the average age of the patients was 54.9 years (SD +15.4), including 107 men and 97 women. The average time from symptom onset to hospital admission was 8.1 days (SD +4.9).
- Patients with digestive symptoms had a significantly longer time from onset to admission than patients without digestive symptoms (9.0 days versus 7.3 days). This may indicate that patients presenting with digestive symptoms sought care later because they did not yet suspect COVID-19 in the absence of respiratory symptoms, like cough or shortness of breath.
- Patients with digestive symptoms had a variety of manifestations, such as anorexia (83 [83.8%] cases), diarrhea (29 [29.3%] cases), vomiting (8 [0.8%] cases), and abdominal pain (4 [0.4%] cases).
- Seven patients with COVID-19 presented with digestive symptoms but no respiratory symptoms.
- As the severity of the disease increased, digestive symptoms became more pronounced.
- Patients without digestive symptoms were more likely to be cured and discharged than patients with digestive symptoms (60% versus 34.3%).
- Laboratory data revealed no significant liver injury, although other studies have shown signs of liver involvement; more research is required to understand the impact of COVID-19 on liver function.
Things to Think About
Given the information from this particular study, it's important to pay attention to the fact that anorexia was in 83.8% of patients tested.
If you leave out anorexia, the percentage of COVID-19 patients with GI symptoms is closer to 30%.
For the overall study population, it ws found that the average time from symptom onset to hospital admission was 8.1 days.
However, it was 9.0 days for patients with GI symptoms, including those with anorexia, compared with 7.3 days for those who did not have digestive symptoms. Seven patients had digestive symptoms but no respiratory symptoms at admission.
Digestive symptoms appeared to be tied to worse outcomes. Whereas 60% of patients without digestive symptoms recovered and were discharged, only 34.3% of the patients with digestive symptoms recovered.
Why Digestive Symptoms?
The virus enters human cells through the ACE2 receptor in the lungs but also in other body parts, including the GI tract.
We think the virus gets into saliva and we swallow it, and then it passes through the acid layer in some patients and uses the ACE2 receptors to enter epithelial cells that line the intestine.
There is clear evidence from endoscopy that it can damage the stomach and the intestines.
Gut Health Impacts Overall Health
Rather than taking a shit (pun intended) ton of supplements to improve Gut Health and your Microbiome, the food you eat ultimately has the biggest impact on the range and type of microbes in the gut.
A diverse microbiome is a healthy microbiome, containing many different species that each play their part in immunity and health.
Microbiome diversity declines as you get older, which may help to explain some of the age-related changes we see in immune responses, so it’s even more necessary to maintain a healthy microbiome throughout life.
The fine details of the interactions between the gut microbiome and the immune system are not fully understood.
But there seems to be a link between the makeup of the microbiome and inflammation – one of the hallmarks of the immune response.
Gut bacteria produce many beneficial chemicals and also activate vitamin A in food, which helps to regulate the immune system.
The best way to increase microbiome diversity is by eating a wide range of plant-based foods, which are high in fiber, and limiting ultra-processed foods including junk food.
If you are concerned about getting hold of fresh produce while self-isolating or quarantined, frozen fruit, berries and vegetables are just as healthy as their fresh counterparts and will last much longer than the currently recommended two-week isolation period.
Canned fruit, beans and pulses are another long-lasting option.
You can also support your microbiome by regularly eating natural yogurt and artisan cheeses, which contain live microbes (probiotics).
Another source of natural probiotics are bacteria and yeast-rich drinks like kefir (fermented milk) or kombucha (fermented tea).
Fermented vegetable-based foods, such as Korean kimchi (and German sauerkraut) are another good option.
Finally, there are a few digestive health supports that you can consider to optimize your overall health.