How Statin Drugs Work
Your liver produces cholesterol through a pathway called the mevalonate pathway – that involves an enzyme HMG-CoA reductase.
Statin drugs block the production of this enzyme and lower the cholesterol production in the liver.
The picture below shows the entire process.
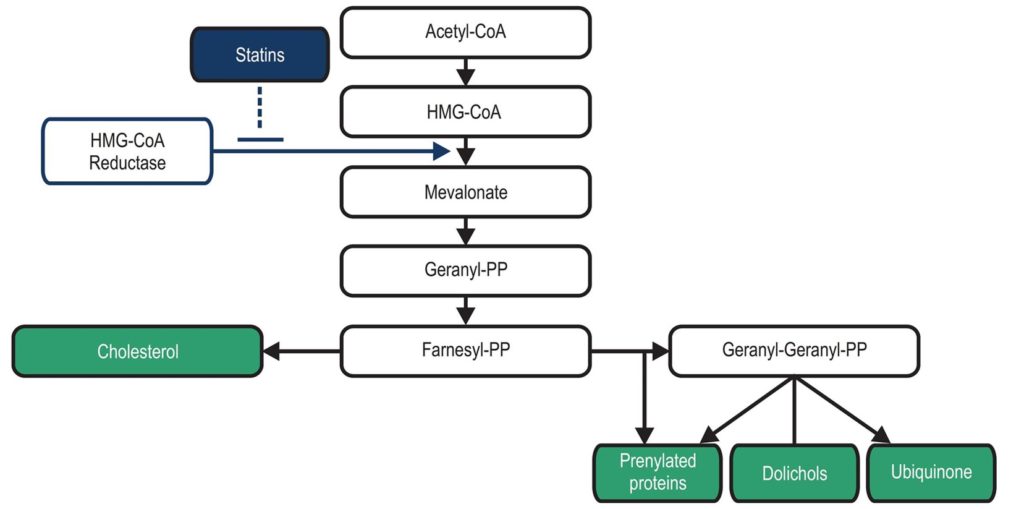
However, things don’t end here.
Besides cholesterol, the mevalonate pathway (with the enzyme HMG-CoA reductase present at the base of it all) is also involved in the production of other non-sterol compounds such as CoQ10 (ubiquinone), dolichols, heme-A, selenium containing proteins, sex hormones such as Estrogen, Progesterone and Testosterone, stress hormones such as cortisol, bile acids important for digestion and vitamin D. [1]
So, when you are using statin drugs, you are not only lowering your cholesterol levels but also disrupting the production of so many other compounds that are essential for cell growth, and maintain heart, muscles, brain and immune health.
Do Statin Drugs Really Work?
Well, statin drugs do what they are meant to do; they lower your cholesterol levels.
So Yes, statin drugs work.
But does this mean you are getting any healthier?
Does it mean that your risk of getting heart disease or having a stroke is decreased?
Does it mean you'll live longer?
The answer is NO!.
In a previous article, we discussed the importance of cholesterol in the body and that lowering cholesterol has no real significance on your heart health.
On the other hand, there is a plenty of evidence that statin drugs come with many serious side effects.
We will talk about these side effects in details, but first, it is time to address the most controversial question.
Do Statins Prevent Heart Disease?
First, it is important to know that your cholesterol levels play a minor role, if at all, when it comes to your risk of developing heart disease or getting a heart attack.
Chronic inflammation (prompted by tissue damage, stress and excessive consumption of sugar and processed foods) contribute much more to this risk.
So cholesterol by itself is not the issue. But elevated cholesterol with tissue damage, excessive stress and too much sugar is a bad combo.
Doctors like to blame cholesterol because it is found at the site of inflammation, injury and damage.
But that is only because cholesterol itself is an anti-oxidant and anti-inflammatory compound.
Which actually begs the question, “Why lower it?”
Cholesterol is also easy to blame because you can significantly lower it by using medications (and it makes a lot of money).
Secondly, evidence suggests that statins may actually increase your risk of developing heart disease and heart problems.
Research and clinical trials prove that taking statins is nothing sort of a gamble – only favorable in some patients and under narrow circumstances.
That brings us to the use of statins in primary prevention and secondary prevention.
Statin Drugs in Primary Prevention: Low Risk Patients
A study examined the effect of statins in people who have never suffered a heart attack or stroke; which is mostly the case as statin drugs are commonly prescribed at the first sign of elevated cholesterol.
Not surprisingly, the analysis found that statins do lower cholesterol in most of these people, but only a very few people will dodge a cardiovascular event (a heart attack or a stroke) because of statins.
More specifically [2]:
- 1 in 60 (1.6%) prevented a heart attack
- 1 in 268 (0.4%) prevented a stroke
- 1 in 67 (1.5%) developed diabetes
- 1 in 10 (10 %) suffered from muscle damage
In addition, statins don’t extend or have any significant impact on lifespan.
A 2010 meta-analysis of the clinical trials examined whether stains have any effect on longevity in a high-risk primary prevention scenario.
The study found that statin therapy does not significantly reduce all-cause mortality risk among high-risk people without any with clinical history of coronary heart disease. [3]
Statin benefits are obviously overstated!
In 2015, a study published in Expert Review of Clinical Pharmacology indicated that both the safety and life-saving ability of statin drugs have been exaggerated.
The researchers stated that statins effectively reduce cholesterol levels, but do not offer any impressive cardiovascular disease outcomes, also adding that statin researchers use ‘statistical deception' to embellish claims about their effectiveness. [4]
For example, statins actually benefit only 1% of the population; meaning these drugs will prevent a heart attack in only one out of 100 patients.
This is the absolute risk.
But this figure is certainly not presented as is, but by using another statistic called the ‘relative risk’.
This results in creating an illusion that statins prove effective in 30-50% of the population.
The study authors, Dr. David M. Diamond and Dr. Uffe Ravnskov explained further “In the Jupiter trial, the public and healthcare workers were informed of a 54 percent reduction in heart attacks, when the actual effect in reduction of coronary events was less than 1 percentage point.”
That's statistics for ya!
“In the ASCOT-LLA study, which was terminated early because it was considered to have such outstanding results, there were heart attacks and deaths in 3% of the placebo (no treatment) group as compared to 1.9% in the Lipitor group.
The improvement in outcome with Lipitor treatment was only 1.1 percentage point, but when this study was presented to the public, the advertisements used the inflated (relative risk) statistic, which transformed the 1.1% effect into a 36% reduction in heart attack risk.” [5]
John Abramson, MD (of Harvard Medical School and author of Overdosed America), and James Wright, MD (of University of British Columbia) analysed 8 clinical trials on the effect of statins versus placebo.
They reported in the journal Lancet that the absolute risk reduction of 1.5% is insignificant. [6]
The analysis further suggested that:
- Statins should not be prescribed in women of any age or for men older than 69 years (as a primary prevention.)
- Men considered high risk and aged 30-69 years should be counselled that about 50 patients need to be treated for 5 years to prevent one cardiovascular event.
- Clinical data do not support the use of statin therapy in primary cardiovascular prevention.
On the other hand, plenty of evidence points to the fact that statins actually “augment cardiovascular risk in women, patients with Diabetes Mellitus and in the young”. [7]
So all that said, statins can work – for a small, select group of patients.

Statin Drugs in Secondary Prevention: High Risk Patients
Studies suggest that statins are effective in people who already have had heart attacks or cardiovascular events.
However, even for this set of population the efficacy of statins is not very remarkable.
As this analysis showed, 5 years of daily statin treatment could only save 1 out of 83 people.
The therapy prevented stroke in 1 out of 125 people and prevented non-fatal heart attack in 1 out of 39 subjects.
At the same time, use of statins over this period caused diabetes in 1 out of 5 people and muscle damage in 1 out of 10 people. [8]
But how do you know where to draw the line?
Let’s simplify this.
Statins can be beneficial in some patients with pre-exiting history of developing coronary heart disease, that is when used a secondary prevention.
This is where the potential risk is quite high.
But if you fall in the low-risk category with no prior history of a heart problem, proceed with caution.
Again, it pays to remember that cholesterol is not a causative factor in heart disease and trying to lower it by using statins, especially in elderly and women, is simply unwarranted.
Consult an expert healthcare professional to help you understand your benefits and associated risks, and decide if the gamble is worth.
Statins are beneficial, even needed, if you have familial hypercholesterolemia.
Familial hypercholesterolemia is a serious genetic condition where the affected person has high levels of blood LDL cholesterol.
Here, the body is not naturally equipped to remove excess LDL from the blood.
The condition is present at the time of birth and can cause heart attack and other cardiovascular problems at quite an early age.
Are Side Effects of Statins Worth the Risk?
Statins exert a wide range of adverse effects that more than offset the modest benefits.
Revisiting the 2015 study by Diamond and Ravnskov, the authors stressed that cholesterol lowering consequence of statins is often associated with an increased risk of cancer.
They also highlighted that most statin trials are concluded within a span of two to five years.
This period is not long enough to record the development of most cancers.
Coming back to the question: Do Statins Really Prevent Heart Disease?
On the contrary. Let’s find out.

Statins and Heart Disease Risk
A 2015 study published in Expert Review of Clinical Pharmacology showed that statins may actually trigger atherosclerosis and heart failure.
The study highlighted various mechanisms to show statins may aggravate your heart problems and concluded that statins work as mitochondrial toxin that “impair muscle function in the heart and blood vessels through the depletion of coenzyme Q10 and ‘heme A', and thereby ATP generation.” [9]
Let’s take a look.
Statins supresses CoQ10 production
Statin drugs target mevalonate pathway to control cholesterol production. But this important pathway is also involved in the synthesis of CoQ10 – a coenzyme present in every cell of the body.
CoQ10 plays an indispensable role in the production of ATP, the energy currency, in the mitochondria.
Without CoQ10, our body won’t be able to produce any bit of energy.
The co-enzyme is also a powerful anti-oxidant and protects the arteries from oxidative damage and ensuing inflammation.
It is easy to see how these properties translate into heart health benefits?
Your heart needs the maximum energy funding to continue beating nonstop – pumping oxygen and nutrient-rich blood across the body.
This is the precise reason why heart has the highest concentrations of CoQ10 as compared to any other organ in your body.
Now, statin drugs deplete your body of CoQ10.
Low CoQ10 levels, especially in the heart, contribute to the onset and progression of congestive heart failure (CHF) and heart attack.
Statins and muscle pain
Statins have adverse effects on skeletal muscle – ranging from mild muscle pain, muscle fatigue to more serious rhabdomyolysis.
Statin drugs inhibit the production of CoQ10 levels, an action that impairs the energy production in the muscles.
This causes muscle weakness and fatigue.
A 2013 study concluded that musculoskeletal conditions, arthropathies, injuries, and pain are more common in people who are on statins than non-users.
The study explained that among other factors, the blocking effect of statins on the synthesis of COQ10 as well as the selenoproteins may be at play here. [10]
Selenoproteins such as glutathione peroxidase play a pivotal role in averting oxidative damage in the muscle tissue.
One rare, but extremely dangerous, side effect of statins is a condition called rhabdomyolysis.
In this condition, damaged muscle tissues break-down and release a protein called myoglobin into the bloodstream.
Too much of myoglobin in the blood can cause damage to the kidneys.
The most telling symptoms of rhabdomyolysis include intense muscle pain throughout the body, muscle weakness, dark colored urine and general feeling of being sick.
The risk of rhabdomyolysis increases with the increased dose of statins.
Statins block vitamin K2 synthesis
Statins inhibit the production of vitamin K2.
The vitamin is known to mobilize calcium into the bones and keep it away from arteries and soft tissues – thus preventing calcium deposition and build-up of plaque in the arteries.
Vitamin K2 activates matrix Gla-protein, that prevents calcification in the arteries. [11]
Vitamin K2 also activates osteocalcin – a protein that holds onto calcium and directs it towards the bones – making bones stronger and less prone to fracture.
Statins May Cause Cognitive Decline
It is simple.
Your liver makes cholesterol because the body needs it for so many things (to make vitamin D, bile acids and all kinds of important hormones).
When your cholesterol levels drop too low, as with long-term and high dose statin users, your body would seek it from other cholesterol-rich sources, for example the brain.
Your brain contains about 25% of the cholesterol in the body.
It plays a critical role in the transmission of neurotransmitters and facilitates communication between the neurons, which helps us to think and affects how well we learn new things and make memories.
When cholesterol dips too low in the brain, a lot of patients on statins suffer memory loss and decline in their cognitive abilities.
We know that statins work by reducing cholesterol production in the liver.
A 2009 research by Yeon-Kyun Shin, an Iowa State University scientist, demonstrated that statins may also keep the brain from synthesizing cholesterol.
Shin tested how the release of neurotransmitters by the brain cells is affected both in the absence and presence of cholesterol.
When he measured the protein function in the brain with cholesterol in attendance, there was a five-fold increase in the protein function.
Shin further explained that cholesterol alters the shape of the protein to stimulate thinking and memory. [12]
In 2009, a research published in the Journal of Lipid Research concluded that “the long-term effects of statin therapy could lead to transient or permanent cognitive impairment in patients who already have low levels of brain cholesterol.” [13]
This is a huge cause of concern in the elderly because with age, there is a lot less production of cholesterol in the brain already.
In addition, cholesterol as well as phospholipid levels are reduced in the patients with Alzheimer’s Disease.
The study showed that statins influence the expression of genes involved in neurodegenerative processes and suggested a potential mechanism that triggers statin-induced cognitive impairment in vulnerable patients.

Statins Increase the Risk of Diabetes
Statins increase your risk of diabetes through many mechanisms.
Studies show that long-term statin therapy increases the risk of new-onset diabetes, possibly by damaging the functions of pancreatic beta cell and by reducing insulin sensitivity. [14] [15]
In addition, statins elevate blood sugar levels.
The drugs also inhibit the production of CoQ10, a nutrient that helps to control blood sugar levels.
Finally, the British Medical Journal published a scientific paper demonstrating that higher potency statins were associated with an increased risk of new onset diabetes.
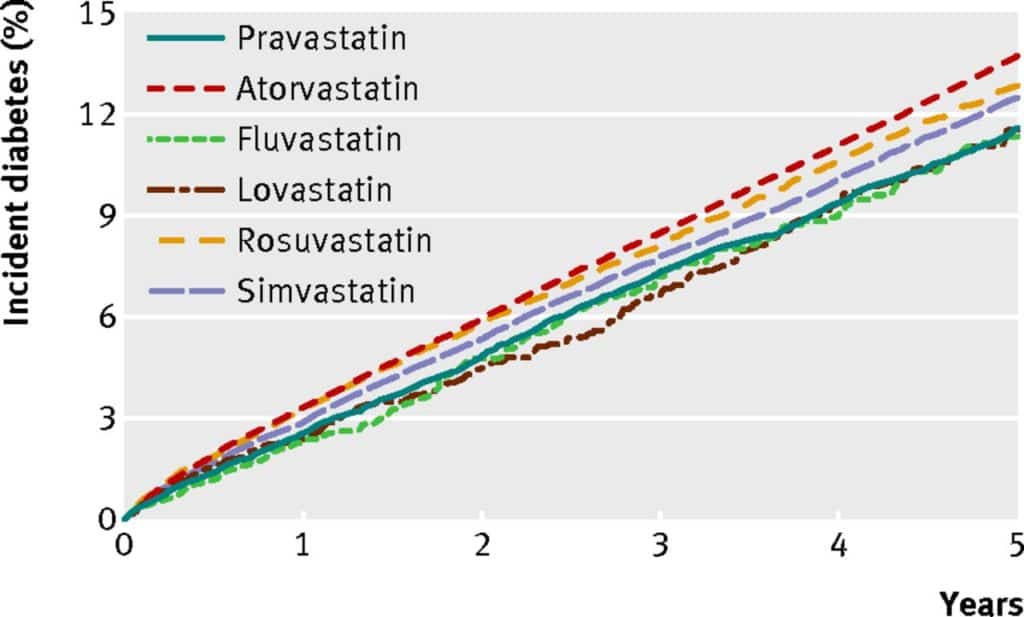
Statins Increase the Risk of Developing Cataracts
Cataract, the cloudiness in the eye lens, is a leading cause of reduced or blurred vision among the elderly.
It is primarily caused by oxidative damage induced by free radicals.
Studies show that statins increase the risk of developing cataracts. [16]
A recent 2016 study hinted at the possibility that increasing use of statins could be contributing to “rising rates of cataract surgery.” [17]

So Are Statins Any Good?
Yes, statins do lower cholesterol levels but this outcome does not translate into any significant cardiovascular protection, especially in people without any history of coronary heart disease.
Statins are effective in reducing heart attacks and death (from heart disease) in people with existing heart problems; especially in middle aged males.
Statins shouldn’t be prescribed to elderly people or to women.
People with active liver disease should not be prescribed statins.
Pregnant and breast-feeding women should not take statins.
Statins are extremely dangerous for children in particular, except in familial hypercholesterolemia (a rare genetic condition).
Statins may have anti-inflammation properties but they don’t influence the size of cholesterol particles.
So, what should you do when you are diagnosed with elevated cholesterol?
Making lifestyle changes is a safer and much more effective approach over pharmaceutical interventions.
This is the single most important method to reduce the oxidative stress and bring down inflammation – thus lowering your risk of cardiovascular problems.
Needless to say, lifestyle modifications (such as weight loss, eating right, maintaining blood sugar levels and refraining from smoking) also improve overall quality of life.