Understanding Blood Sugar
There are several terms and concepts that we need to understand before proceeding with how blood sugar can prevent fat loss.
Let's discuss some basic terminology:
- Glucose (blood glucose) – a monosacharide or simple sugar that is the preferred source of energy for our body
- Glycemic – referring to glucose
- Glycemic Index – how fast a food causes your blood sugar to spike
- Glycemic Load – how much blood sugar and insulin is ultimately released by the food we eat
- Glycogen – glucose that is turned into “stored energy” used during physical activity
- Insulin – the primary hormone that moves blood sugar into the cells
- Insulin Sensitivity – the rate at which cells “listen” to insulin
- Insulin Resistance – when the cells stop “listening” to insulin
- Insulin Index – the amount of insulin released by food
Glucose is the preferred source of energy for the brain and a primary source of energy for all cells.
You get glucose by consuming foods.
Glucose is created in plants via photosynthesis and it is largely abundant in carbohydrates.
The primary macro-nutrients that we consume via food can be categorized as
- Proteins
- Carbohydrates
- Fats.
Proteins and are made up of sequences of amino acids. They help to produce antibodies to fight off infections, enzymes to help our biochemistry and act as messengers such as hormones.
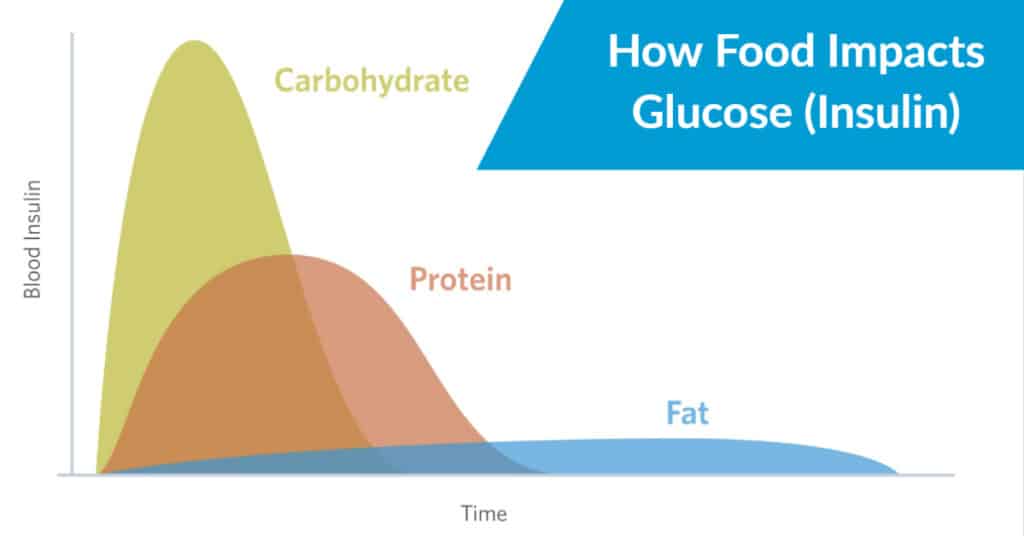
Fats consist of essential fatty acids, triglycerides and cholesterol and act as energy storage molecules, insulation for our organs and they can act as messengers to help proteins do their job. Generally speaking, fats have a nominal impact on blood sugar.
Carbs are by far the most abundant source of glucose that we consume via food.
Carbohydrates can come in the form of simple carbohydrates (processed food, refined flour, sugar, crackers, chips, candy, etc.) or complex carbohydrates (vegetables, fruits, starchy plants and tubers)
Simple carbohydrates have the biggest impact on blood sugar levels.
Some foods cause a rapid rise in glucose (glycemic index) and some foods will cause glucose to stay high over time (glycemic load).
Carbs that have a high glycemic index and high glycemic load will ultimately cause insulin to be high.
However, proteins and fats can increase insulin as well.
This is where the insulin index comes in handy.
In other words, what foods cause a dramatic spike or increase in Insulin?
Ultimately, increasing glucose in the blood stream increases Insulin.
Insulin is the master sugar regulating hormone and can also negatively impact other parts of our body.
High insulin can increase inflammation, cortisol and blood glucose creating a vicious cycle of damage.
The Ups and Downs of Blood Sugar
To make things simple, there are 2 primary ways that you can have blood sugar imbalances causing major problems for the body.
And if there are imbalances or dysfunctions in blood sugar regulation, optimal health and fat loss are nearly impossible.
The two primary types of blood sugar problems include:
- Chronically elevated blood sugar – characterized by elevated glucose levels and elevated insulin
- Blood Sugar Fluctuations (Dysglycemia) – which refers to low blood sugar but can be characterized by fluctuations of high and low blood sugar.
The problem is that both of these states result in insulin surges, which is what we ultimately want balanced.
Insulin takes blood sugar and stores it as fat.
Insulin does this because blood sugar becomes a problem at extreme levels – whether its high or low.
This is why the body takes such extreme measures to maintain normal glucose levels in the body.
And the primary way of doing that is through the usage of insulin.
High Levels of Blood Sugar

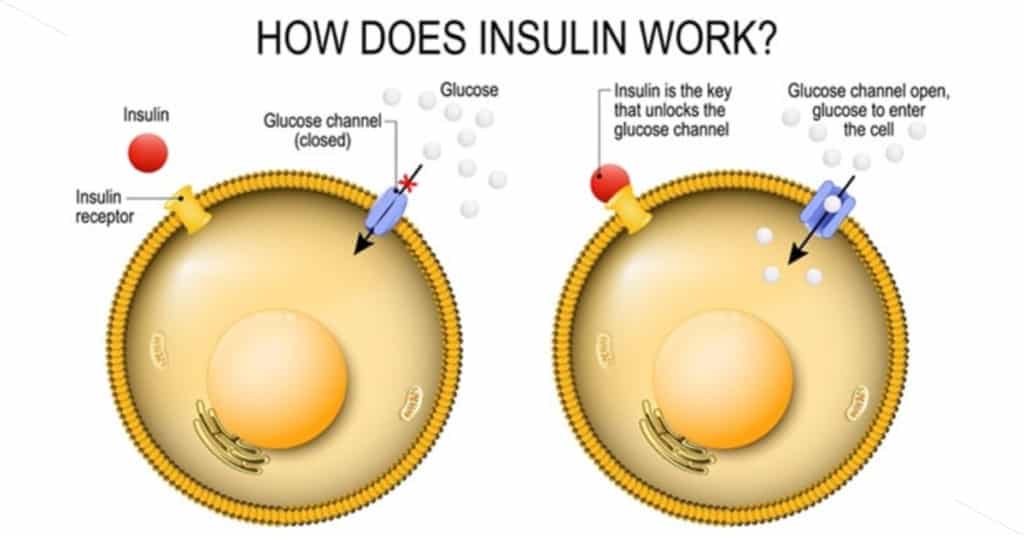
When blood sugar is released into the blood stream, the body will secrete insulin.
Insulin’s primary goal is to get the sugar from our blood into our cells where they can use it for energy.
This is why low energy is one of the early warning signs of insulin resistance.
Insulin helps sugar get into our cells by connecting with specific insulin receptors on the cell wall, which then opens the doors of our cells to let sugar in.
A very important question to ask is, “What happens when sugar is always present and insulin is always high?”
Well our cells start to reduce the number of receptors, or doors, that let sugar inside of the cell.
If there's always insulin present, then the cells don't need as many doors.
With less doors to open to let glucose inside, insulin starts to increase and so does sugar, and this is what we call Type 2 Diabetes.
That's why Type 2 Diabetes is characterized by elevated glucose and insulin.
So when someone follows a poor quality diet or a high quantity diet, blood sugar rises beyond healthy ranges and this in turn causes insulin to constantly be circulating.
Eventually the cells become less sensitive to insulin and we call this insulin resistance.
This results in even larger amounts of sugar circulating in the blood, and even larger amounts of insulin.
These elevated levels of blood glucose end up getting stored as triglycerides and fat, which is just one of the many ways that elevated blood sugar makes it difficult to lose fat.
Low Levels of Blood Sugar

The second way that blood sugar can cause issues is when you have chronically low blood sugar or reactive hypoglycemia.
Low blood sugar or major fluctuations in blood sugar throughout the day can be just as damaging as high blood sugar.
When people fluctuate between high and low blood sugar, we refer to this as Dysglycemia.
This condition is harder to evaluate and somewhat elusive to clinicians because they’re not looking for it, or just concerned with elevated glucose.
For this reason, the true incidence of dysglycemia is unknown, but I find it quite a bit when I’m working with patients in my Functional Medicine practice.
Besides the unwanted symptoms of reactive hypoglycemia including irritability, tremors, inability to concentrate and light-headedness, the negative impacts of low blood sugar on fat loss is due to the same thing that makes elevated blood sugar undesirable – insulin.
Why Insulin is Harmful
There is a major misconception running around that diet and exercise are all you need to do to be healthy.
Certainly a healthy diet and regular exercise are a requirement for health, but it’s not ALL you have to do.
The problem is, most humans walking around have caused physiological and biochemical damage that diet and exercise alone cannot correct.
In fact, looking healthy and having a muscular body does not mean you’ll have normal blood sugar.
I know plenty of lean, six pack ab wearing humans who have major physiological problems to the point of serious health condition including kidney failure and autoimmunity.
Researchers are even starting to use terms such as “skinny fat” or “non obese insulin resistance” because normal looking people have blood sugar problems.
When it comes to insulin surges, there are 3 major connections:
- Inflammation
- Cortisol
- More Blood Sugar
Though there are a number of mechanisms involved in this cycle, let’s go over a few basics.
- Elevated blood sugar results in increases in insulin (to remove the glucose in the blood)
- Elevated insulin stimulates the production of inflammatory chemicals and stress hormones
- Both inflammatory chemicals and cortisol cause:
- Increase in heart rate, blood pressure, cholesterol, clotting factors, protein/muscle breakdown
- All of this causes even more blood sugar to be released creating a cycle of blood sugar-insulin-inflammation-cortisol
People will enter this vicious cycle in one of two ways.
The first is through improper eating.
This includes the consumption of excess sugar or carbohydrates, excessively large meals or glycemically imbalanced meals.
The second way is through cortisol.
Anything that elevates cortisol (i.e. stress, infection, food allergies, inflammation, etc.) will also elevate blood sugar and therefore insulin levels.
In other words, you could have a perfect diet and exercise program, but if your HPA-Axis is dysfunctional or you have cortisol problems, your body is releasing excess sugar without food.
How Blood Sugar Impacts Fat Loss

The primary reason why blood sugar impacts fat loss is because of insulin surges or dysregulation.
The more insulin sensitive you are, the leaner you’ll be.
The more insulin resistant you are, the more fat you’ll carry.
While insulin is necessary to sustain life, in excess it has numerous devastating impacts on our body, including making fat loss difficult.
When blood sugar is chronically elevated, insulin levels are chronically elevated.
However, in cases of major sugar fluctuations or dysglycemia, the body will produce periods of high insulin, followed by periods of low.
Both chronically elevated insulin and high/low insulin bursts have many negative metabolic effects, especially as it pertains to fat loss.
First, insulin will create hormonal shifts in both men and women.
In men, insulin will upregulate an enzyme called aromatase, which converts testosterone to estrogen.
Estrogen in men, in addition to being a cardiovascular risk marker, makes it very difficult to lose fat.
On the other hand, elevated insulin in women results in an increase in testosterone production which, in addition to being a cardiovascular risk for women, also makes fat loss very difficult.
Second, insulin stimulates a pro-inflammatory chemical called interleukin-6 or IL-6. IL-6 has a number of damaging effects on the body, one of which includes raising cortisol.
One of cortisol’s primary effects on the body is to increase blood sugar levels, which of course further elevates insulin.
Third, elevated insulin has been shown to create alterations in leptin, a hormone that helps us to feel full or not hungry.
When leptin levels rise, just like any hormone, desensitization occurs and the cells stop listening to leptin.
This creates leptin resistance and makes it very hard for people to stop eating.
Next Steps
The first thing to do is check symptoms.
For example, do you get fatigue after meals?
Do you have a difficult time falling asleep?
Do you get jitters when you go long periods without food?
Do you get headaches or find that you have to get up in the middle of the night quite often?
The next thing to do is get a good quality blood chemistry panel that is also interpreted by someone who really understands how to read blood chemistry from a functional perspective.
Blood sugar issues are far more common than you think, even in “healthy” people.
Here’s the optimal ranges for blood sugar markers necessary to assess blood sugar balance:
- Fasting Glucose – 75 – 86 mg/dl
- Hemoglobin A1C – 4.6 – 5.5%
- Fasting Insulin – 2.0 – 5.0 iu/ml
- C-Peptide – 1.1 – 2.1 ng/ml
- Fructosamine – 190 – 228 umol/L
- Glycomark – values greater than 14 are ideal
- LDH – 140 – 200 iu/L
- ALT:AST Ratio – .10 – .78
If you want something different, consider working with a qualified Functional Medicine practitioner.
Want to speak to a functional medicine professional about increasing wellness?
Book a free 15-minute consultation with Dr. Daniel.